Tramadol Guide
What Is Tramadol and How Does It Work?
Introduction – What is Tramadol
Tramadol is a widely prescribed medication used for the management of moderate to moderately severe pain. It is often considered when over-the-counter pain relievers such as ibuprofen or acetaminophen are not effective enough. Although tramadol is classified as an opioid analgesic, it has a unique mechanism of action that distinguishes it from traditional opioids like morphine or oxycodone.
Understanding how tramadol works, when it is prescribed, and what risks are associated with its use is essential for both patients and caregivers. This comprehensive guide explores the pharmacology, uses, benefits, side effects, and safety considerations of tramadol in detail, helping readers make informed decisions under medical supervision.
What Is Tramadol?
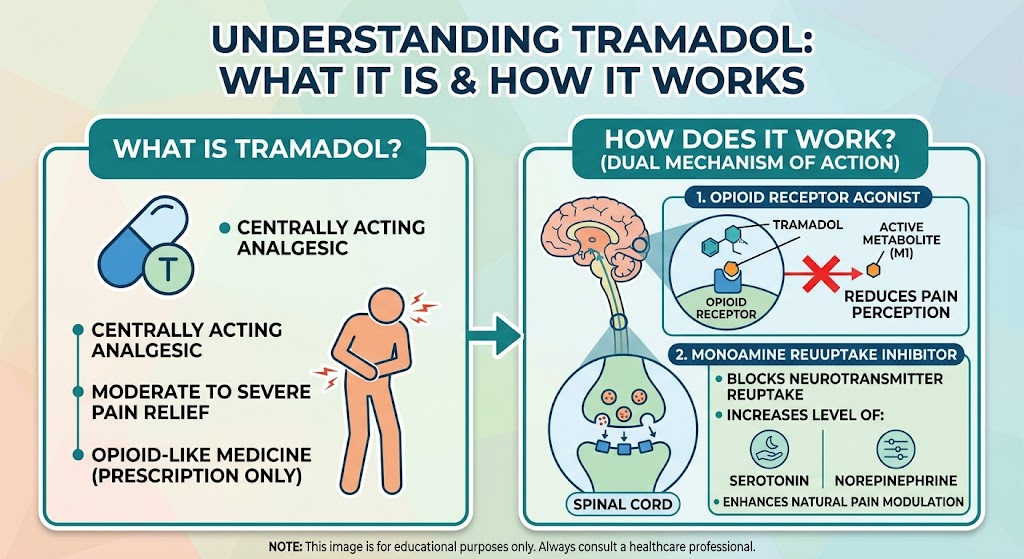
Tramadol is a centrally acting synthetic analgesic that alters the way the brain perceives and responds to pain signals. It is commonly prescribed for acute pain following surgery or injury, as well as chronic pain conditions such as osteoarthritis or neuropathic pain.
Unlike many stronger opioids, tramadol is often positioned as a step between non-opioid painkillers and more potent narcotics. However, despite its relatively moderate strength, tramadol still carries significant risks, including dependence and adverse neurological effects, which require careful medical oversight.

How Does Tramadol Work in the Body?
The effectiveness of tramadol lies in its dual mechanism of action, which involves both opioid and non-opioid pathways. This combination allows it to provide pain relief in a way that is different from many other analgesics.
Opioid Receptor Activity
Tramadol binds to mu-opioid receptors in the brain and spinal cord. These receptors are part of the body’s natural pain control system. When activated, they reduce the transmission of pain signals and alter the emotional response to pain, making discomfort feel less intense.
However, tramadol’s affinity for these receptors is weaker compared to traditional opioids, which is why its effects are generally considered milder.
Neurotransmitter Reuptake Inhibition
In addition to its opioid activity, tramadol inhibits the reuptake of serotonin and norepinephrine, two neurotransmitters involved in mood regulation and pain perception. By increasing the availability of these chemicals in the brain, tramadol enhances its pain-relieving effects.
This dual action is particularly useful in certain types of pain, such as nerve-related pain, where standard opioids may be less effective.
Pharmacokinetics: How the Body Processes Tramadol
After oral administration, tramadol is absorbed through the gastrointestinal tract and metabolized in the liver. One of its metabolites is more potent than the parent compound, contributing significantly to its analgesic effects.
The onset of action for immediate-release tramadol typically occurs within one hour, while extended-release formulations are designed to provide consistent pain relief over a 24-hour period. The drug is eventually excreted through the kidneys, making renal function an important consideration in dosing.
Medical Uses of Tramadol
Tramadol is prescribed in a variety of clinical situations where moderate to moderately severe pain is present. It is not usually the first-line treatment for mild pain but becomes relevant when other medications fail to provide adequate relief.
Acute Pain Management
Tramadol is frequently used after surgical procedures or injuries where short-term pain control is required. Its relatively fast onset makes it suitable for managing sudden discomfort.
Chronic Pain Conditions
Patients with long-term conditions such as osteoarthritis or chronic back pain may be prescribed tramadol when non-opioid medications are insufficient. In such cases, extended-release formulations are often preferred.
Neuropathic Pain
Due to its effect on serotonin and norepinephrine, tramadol may be beneficial in certain cases of nerve pain, although it is not always the primary treatment choice.
Dosage and Administration Considerations
The appropriate dosage of tramadol varies depending on the patient’s age, medical condition, and response to treatment. Physicians typically start with the lowest effective dose and adjust gradually to minimize side effects.
Immediate-release formulations are usually taken every four to six hours as needed, while extended-release versions are taken once daily. It is crucial that patients follow prescribed dosing schedules carefully, as misuse can lead to serious complications.
Side Effects and Adverse Reactions
Like all medications, tramadol can cause side effects that range from mild to severe. Understanding these effects is important for safe use.
Common Side Effects
Many patients experience mild symptoms such as nausea, dizziness, constipation, headache, or drowsiness. These effects often diminish as the body adjusts to the medication.
Serious Risks
More serious adverse effects include respiratory depression, seizures, and serotonin syndrome, a potentially life-threatening condition caused by excessive serotonin levels. The risk of seizures is particularly notable with tramadol compared to other opioids.
Risk of Dependence and Addiction
Although tramadol is sometimes perceived as safer than stronger opioids, it still has the potential to cause physical dependence and addiction. Long-term use can lead to tolerance, meaning higher doses are required to achieve the same effect.
Withdrawal symptoms may occur if the medication is stopped abruptly. These can include anxiety, sweating, insomnia, and flu-like symptoms. For this reason, discontinuation should always be managed under medical guidance.
Safety Warnings and Precautions
Tramadol must be used with caution in several populations. Individuals with a history of substance use disorder, respiratory issues, or neurological conditions should discuss risks thoroughly with their healthcare provider.
Combining tramadol with alcohol, sedatives, or certain antidepressants can increase the risk of dangerous side effects, including slowed breathing and serotonin syndrome. Patients should always inform their doctor of all medications they are taking.
Who Should Avoid Tramadol?
Certain groups may be advised against using tramadol. These include children under 12 years of age, individuals with severe respiratory depression, and patients with uncontrolled epilepsy. Pregnant or breastfeeding individuals should only use tramadol if clearly recommended by a healthcare professional.
Comparison with Other Pain Medications
Tramadol occupies a middle ground between non-opioid analgesics and strong opioids. While medications like ibuprofen are effective for inflammation and mild pain, tramadol provides stronger relief without reaching the potency of drugs like morphine.
However, this does not mean it is risk-free. Its unique pharmacological profile introduces its own set of considerations, particularly related to neurological effects.
Frequently Asked Questions
How long does tramadol take to work?
Immediate-release tramadol typically begins to relieve pain within 30 to 60 minutes, with peak effects occurring within a few hours.
Is tramadol safe for long-term use?
Long-term use may be appropriate in certain chronic pain conditions but requires careful monitoring due to the risk of dependence and side effects.
Can tramadol be taken with other medications?
Tramadol can interact with many drugs, especially those affecting serotonin levels. Medical advice is essential before combining treatments.
Does tramadol cause drowsiness?
Yes, drowsiness is a common side effect, and patients are advised to avoid driving or operating heavy machinery until they understand how the medication affects them.
Conclusion
Tramadol is a versatile and effective medication for managing moderate to moderately severe pain. Its dual mechanism of action allows it to address pain through both opioid receptor activation and neurotransmitter modulation. However, this same complexity also introduces risks that must be carefully managed.
Safe use of tramadol depends on proper medical guidance, adherence to prescribed dosages, and awareness of potential side effects and interactions. When used responsibly, it can play a valuable role in pain management, but it is not without significant considerations.